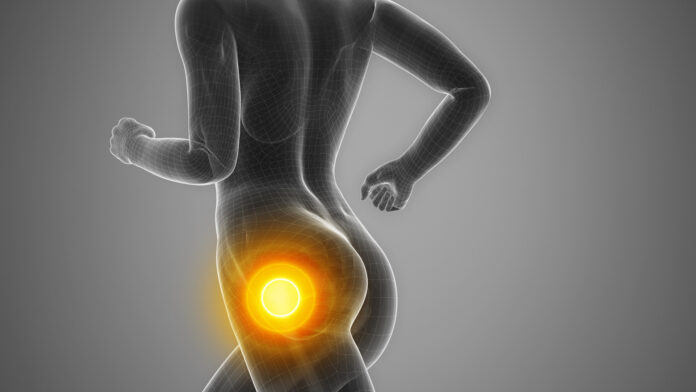
The piriformis is a small muscle, but it holds a reputation for being a big pain in the behind! This thin, triangular muscle lies deep in the buttocks, beneath the much larger gluteus maximus. The piriformis, in concert with other deep hip muscles such as the gluteals, help us to both rotate and stabilize our hips. For runners, these muscles act like the keel or rudder of a boat, countering rotation and lateral forces to keep you moving efficiently over your feet.
There are a lot of anatomical structures surrounding the piriformis, including blood vessels and nerves. The sciatic nerve (which “sciatica” refers to) runs through the buttocks and down the leg, just behind the piriformis. In a small percentage of people, the sciatic nerve runs directly through the piriformis.
“Piriformis syndrome” involves pain in the buttock, sometimes accompanied by sciatica (pain, sensory changes or weakness that radiates down the leg). Frequently, sciatica from the piriformis is confused with sciatica from the lower back. While sciatica affects approximately 20 per cent of people over the course of their lifetime, true piriformis syndrome is a relatively rare cause of sciatica, accounting for about seven per cent of cases. People with piriformis syndrome often have difficulty with tasks involving force transmission through the pelvis (running, stair climbing, or even sitting). Runners may experience symptoms of piriformis syndrome after a significant change to their running load.
TREATMENT OPTIONS
Soft tissue Management
Massage and/or dry needling (IMS) can loosen taught bands of the muscle, helping to restore the proper extensibility of the muscle and release myofascial trigger points that may be present. Neurodynamic stretching or “flossing” has also shown good research support; this exercise can help limit compression of the sciatic nerve in the piriformis area.
Exercise Progression
After severe symptoms settle, exercise for piriformis syndrome should focus on strengthening the hip, pelvis, and core muscles. These regions all depend on each other to absorb shock and propel us forwards efficiently. There is particularly strong evidence to support strengthening the hip abductor and external rotators.
One case study on a basketball player with Piriformis syndrome focused on progressive exercise in three phases, with excellent results. The first phase focused on muscle isolation, the second was based on weight bearing exercise, and the last focused on dynamic loading such as running, jumping, etc. (See exercises related to running below). The athlete went from having 9/10 pain after playing basketball to 0/10 pain within weeks. After 52 weeks there was no recurrence of pain.
Changes to Running Dynamics
Research has shown that increasing stride rate (the number of times a runner’s feet hit the ground in a minute) by even 10 per cent reduces peak stress on the piriformis muscle by an average of 14 per cent. This can be an easy way to reduce stress on the piriformis, while returning to running.
EXERCISES
A good starting point would be to complete two sets of the following, twice daily. They should not cause pain.
Stretch-band sidestep: Isolation (Phase 1)
Place a looped stretch band just above both knees. Bend hips and knees softly but keep posture upright. Step to one side, keeping some tension in the band, and pointing the feet forwards. Reverse direction once you reach the end of your space, or after 20 reps. Start with one minute. Level up: place the band around the calves or ankles.
3D taps: Weight-bearing loading (Phase 2)
Stand on one leg, with a soft bend in the knee. Reach your non-standing leg out directly to the side, gently tapping the ground at the end of your reach. Return the foot to centre, then reach out to tap diagonally backwards (45 degrees), and finally straight behind you. Avoid letting the standing knee fall inwards and try to keep an even pressure throughout your standing foot. Aim for 12-15 taps on each side. Level up: add a band around the knees.
Quick feet: Dynamic loading (Phase 3 and cadence)
Set a metronome to 180 beats per minute (easy to find on YouTube). Softly run on the spot or move forward slowly, matching your arm swing to your feet. Try to keep an upright posture and aim for one minute of continuous motion.
Piriformis syndrome can slow runners down temporarily, but we have research on our side to keep us moving forward! After settling the pain, we can progressively build strength and stability in the tissues around the hips to “steady the ship.” By building tissue resilience and perhaps increasing cadence, you can become more efficient as a runner. Through better efficiency you can prevent injury and run faster with wind in your sails.

Read This Story in Our 2022 Running Digital Edition
2022 RACE SOURCE GUIDE. Training plans for every distance, yoga for runners, athletes with impact, running in the metaverse, recipes and much more!